Reducing Clinician Burden and Unlocking Value Through AI

Artificial intelligence in healthcare has rapidly moved from hype to practical implementation. At Hackensack Meridian Health (HMH), one of New Jersey’s largest health systems, AI is no longer a futuristic concept but a daily reality that is reshaping workflows, improving patient experience, and supporting clinicians.
In a recent episode of The Big Unlock podcast, Sameer Sethi, Senior Vice President and Chief AI & Insights Officer at HMH, shared how the organization is embedding AI into its core operations. With a portfolio spanning data and analytics, AI, robotic process automation (RPA), and software development, Sameer and his team are focused on one mission—using AI to create real-world impact.
Listen to the full conversation
Moving Beyond Theory: AI in Clinician Workflows
For Sameer, the value of AI lies not in experimental pilots or theoretical discussions, but in embedding technology directly into workflows. “It’s one thing to give someone access to a conversational AI,” he explained. “But the real value is in customizing it for clinicians at the point of care.”
One of HMH’s earliest use cases with large language models was clinical summarization. Traditionally, physicians spend significant time combing through patient records during visits, time that often takes away from patient interaction. By building an AI-powered “summarize” button, clinicians can now generate instant patient summaries. Over time, this tool has evolved to generate specialty-specific summaries for more than 15 clinical disciplines.
The impact has been tangible – less “pajama time” spent completing documentation, reduced cognitive burden, and more meaningful clinician-patient interactions.
Harnessing Patient Feedback at Scale
AI is also helping HMH analyze patient sentiment at scale. Post-discharge surveys often contain rich insights, but unstructured comments are difficult to process manually. Sameer’s team applied generative AI models to perform sentiment analysis across thousands of survey responses.
This approach revealed trends that might have been overlooked, giving unit-level leaders actionable insights. “We’re not just looking at individual comments but synthesizing them in volume,” Sameer noted. “That allows us to surface patterns and improve care delivery.”
Building Trust and Adoption: Governance and Feedback Loops
Sameer emphasized that technology alone is not enough—adoption requires trust. At HMH, clinicians are closely involved in the development process. “We first understand the problem that needs to be solved, then partner with the clinicians who want to solve it,” he said.
Transparency is key. For example, with clinical summarization, clinicians are reminded that AI is not 100% accurate and should be treated as a decision-support tool, not a replacement. This approach helps maintain trust while reinforcing the principle of keeping a “human in the loop.”
Equally important are continuous feedback loops. From simple thumbs-up/thumbs-down ratings to detailed comments, feedback is built into every deployment. “If we don’t capture feedback, adoption eventually suffers,” Sameer explained.
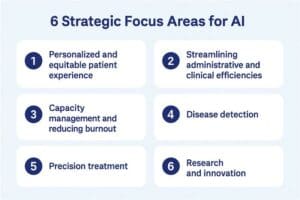
On a broader level, HMH has established a governance “pyramid” that ensures AI implementation aligns with organizational priorities. It starts with technical teams evaluating models, includes a cross-departmental governance group with representatives from legal, HR, finance, and clinical domains, and culminates in oversight by the executive leadership team and board. To channel innovation into meaningful outcomes, HMH outlined six focus areas for AI. Every proposed AI use case is evaluated against this framework, with higher priority given to those that align with multiple focus areas and deliver clear ROI.
Disease Detection and Early Intervention
Unlike many health systems that avoid AI-driven disease detection due to regulatory concerns, HMH has embraced it using machine learning models with minimal risk of “hallucinations.” Sameer shared that disease detection emerged as the top priority during a board vote.
Examples include:
- Mortality Prediction and Palliative Care Nudges: A model predicts a patient’s likelihood of mortality within six months. If triggered, clinicians receive a best practice alert prompting them to consider a palliative care referral. “We’re not making decisions—we’re nudging clinicians at the right time,” Sameer clarified. This approach ensures patients and families receive appropriate support earlier in their care journey.
- Chronic Kidney Disease (CKD) Detection: Early identification of CKD enables timely interventions that can slow progression and improve outcomes.
- Chronic Asthma Prediction: Similar predictive models are being developed to flag patients at risk of asthma complications.
These initiatives underscore Sethi’s philosophy: AI should support clinicians in making informed decisions, not replace their judgment.
The Next Frontier: Agentic AI
When asked about future trends, Sameer response was unequivocal: “Agents. Agents. Agents.”
Agentic AI, he explained, represents the next evolution—where different technologies such as large language models, rule engines, and RPA are orchestrated to perform complex workflows end-to-end.
Take denial management as an example. Traditionally, humans analyze insurance denial letters, identify issues, prepare appeals, and resubmit claims—a time-intensive process that affects cash flow. At HMH, an AI agent now handles much of this sequence:
- Reading and synthesizing denial letters with a language model
- Applying a rule engine to identify missing information
- Drafting an appeal letter with generative AI
- Using RPA to route it to a human for review and submission
By automating most of the process, humans intervene only at the final review stage, dramatically reducing turnaround times and administrative burden.
“This is the evolution of AI,” Sameer said. “Taking insights and moving them into the next step without always relying on a human.”
A Personal Journey into Healthcare
Sameer’s commitment to healthcare is deeply personal. Early in his career, he worked in financial services, while his wife, an occupational therapist, returned home one day and told him, “I made someone walk today. What did you do?” That moment, he recalls, triggered a desire to make a direct impact on people’s lives.
“I realized I could apply my skills in analytics to healthcare and help patients live better—or even die better,” he reflected. Since then, he has remained firmly committed to the field.
Looking Ahead: Data, Capabilities, and Willing Consumers
Sameer is optimistic about the future of AI in healthcare, citing three enablers that did not exist a decade ago:
- Data abundance: From EHRs to wearables, data is now ubiquitous.
- Advanced capabilities: Off-the-shelf models and cloud platforms accelerate innovation.
- Consumer readiness: Patients have become more open to digital care, especially post-COVID.
“Healthcare will always be a people business,” he acknowledged, “but the world—and consumers—are ready for digital means of delivery.”
Sameer’s work at Hackensack Meridian Health highlights a critical shift in healthcare AI: from experimentation to embedded, trusted, and scalable solutions. By focusing on clinician workflows, patient sentiment, governance, and forward-looking technologies like agentic AI, HMH is building a model of AI adoption that balances innovation with responsibility.
As health systems everywhere grapple with clinician burnout, administrative inefficiencies, and rising costs, Hackensack’s approach offers a clear blueprint: start with real problems, keep clinicians engaged, embed AI into workflows, and never lose sight of the human element.
A Pediatric-Centric Approach to AI
Pediatric healthcare comes with its own unique challenges—fewer available data points, smaller population sizes, and higher sensitivities around communication and consent. This makes the responsible use of AI even more critical.
Dr. Morse noted that solutions must be designed with children and families in mind, not simply adapted from adult care settings. Whether deploying ambient tools, summarizing clinical notes, or streamlining administrative workflows, every use case must prioritize trust, safety, and patient experience.





