Healthcare digital transformation
A primer for healthcare executives and technology solution providers

Digital transformation: gaining momentum in healthcare
The critical questions for a healthcare CEO considering digital transformation strategy today are:
- What does “digital” mean to us?
- How do we see it impacting the enterprise in the future?
- What are other leading enterprises investing in and how will that impact our competitive position?
The future of healthcare is in digitally reimagined experiences for patients and caregivers alike. Digitalization offers increased choice and convenience for patients, and improved outcomes for caregivers while reducing costs and workloads.
The explosion of data sources, particularly genomics, wearables, and sensor data, along with advanced analytical capabilities, is enabling new digital health experiences.
Despite the promise, digital transformation in healthcare faces several headwinds. The shift from fee-for-service to value-based care is not as rapid as was expected. Falling reimbursements in an accountable care era lead to diminishing margins for health systems, leaving little for discretionary spending on technology spend for returns in the distant future.
The healthcare sector is in the midst of consolidation, and the threat of disruptive non-traditional players looms large.
Technology and execution risks in enterprise digital transformation remain high due to various factors. Continued underinvestment in technology over the years means that scarce resources are being consumed in addressing technical debt. As incumbents in every sector get disrupted by a tidal wave of digitally enabled competitors, the writing on the wall is clear for many healthcare enterprises – it’s about survival.
As Greg Silvesti, Head of Digital Health & Innovation for AbbVie, puts it: Digital is now cost of entry for organizations looking to play an important role in the future of healthcare.
Key themes in digital transformation
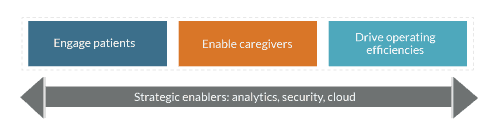
The digital transformation framework above describes at a high level the objectives of a digital strategy. There are three broad focus areas for digital transformation in healthcare today:
- For health systems and health plans, engaging patients and enabling caregivers directly relate to how care will be delivered in the future.
- For pharma and life sciences companies, it may mean focusing on drug discovery processes and introducing digital therapeutics in the way drugs are prescribed and consumed.
- A third focus area is the operations of a healthcare enterprise – how HR, legal, supply chain, and finance can be improved through digitally transformed processes.
According to a report by the American Hospitals Association (AHA) in 2017, more than 65 percent of hospitals have implemented telehealth in at least one care unit, while an additional 13 percent plan to implement telemedicine within the next year.
- The concept of virtual hospital is gaining traction: Intermountain’s virtual hospital Connect Care Pro provides basic medical services as well as stroke evaluation, intensive care, newborn critical care and mental health services.
- The Cleveland Clinic’s Distance Health program includes synchronous virtual visits, e-visits, e-consults, remote image uploads, and eHospital and eICU for remote monitoring of acute care patients.
- Remote monitoring has gained a significant amount of traction as a means to reduce caregiver workload and save costs. Kaiser Permanente has launched Bluetooth-enabled glucose meters to enable patients to have their readings automatically synced to their mobile devices.
The terms digital and digitalization are used interchangeably and often confusingly. Digital refers to technologies that promise to automate and accelerate how a business runs. Digitalization is the integration of digital technologies to reimagine business processes and provide new revenue and value producing opportunities.
A phased approach to digital transformation
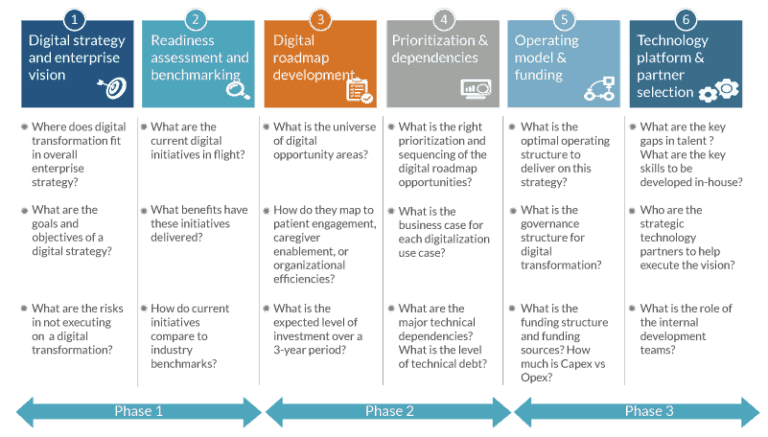
Phase 1: Digital strategy and readiness assessment
The digital transformation journey begins with developing a vision for the enterprise and an assessment of the current maturity level and enterprise-readiness for digital transformation. This starts by addressing fundamental questions about digital aspirations for the enterprise.
A simple categorization such as the one below helps benchmark aspiration levels and align it with enterprise-level expectations.
- Digital pioneer
For enterprises in this category, digital is a top enterprise priority, supported by adequate funding and cross-functional executive sponsorship. These enterprises tend to have a comprehensive digital strategy for the enterprise that goes beyond a narrow focus on telemedicine or process automation. - Digital follower
For these enterprises, digital strategy closely follows that of industry leaders, driven mainly as IT initiative focusing on one or two key areas. Leadership tends to be conservative about innovation programs, and prescriptive about near-term returns on investments. - Digital opportunist
These enterprises do not have a formal digital transformation strategy. Digital investment decisions tend to be driven by market pressures and funding availability and are very often departmental initiatives that operate in isolation. For such enterprises, IT governance is as much a challenge as driving an enterprise-wide IT-led digital strategy.
A self-assessment of readiness levels starts by looking at current in-flight initiatives and the maturity levels of the same. The indicative list of questions below will help establish a baseline to determine strategy going forward.
(We recommend administering these questions via an internal survey)
- Name and describe the digital initiatives currently deployed in the enterprise.
- What have been the achievements of such efforts to date?
- How do you measure success (key metrics)?
- What investment has gone into these programs so far (last 1-2 years)?
- Do you have a view of the future state for your initiative?
- What kind of resources do you need to get to future state?
- Is there a documented business plan/ case for investment? If no: how do you plan to fund your initiative?
- How does your initiative enable new care models or change existing care models?
- What challenges do you foresee in the development and adoption of your initiative?
- Who are your “first adopters”? How will their experience and results be leveraged to accelerate adoption by other users?
- What are the risks associated with your program and how do you plan to mitigate them?
- What internal/ external technology capabilities are required to enable the transformation (or, to implement your initiative)?
Enterprise readiness is another critical factor to consider before launching a program. Readiness assessment requires evaluating current patient and caregiver experiences, the maturity level of support operations, and IT infrastructure readiness. A significant factor in IT readiness is technical debt, which refers to the level of investment required to upgrade the IT infrastructure to meet the digital aspirations of the enterprise.
Other factors include free cash flow for investments, capacity for large-scale change management, and a reliable technology partner ecosystem among other things.
We also recommend reaching out to peers in the sector who have launched digital transformation initiatives, refer to industry research, and engage potential technology and consulting partners in gathering industry insights based on their customer relationships.

Phase 2: Roadmap development and prioritization

A digital roadmap may include a “wish list” of all the possible digital solutions for a healthcare enterprise, and the list may have to be rationalized and prioritized to allow for budget and resource allocations.
The marketplace for ready-to-deploy solutions is also in the early stages of maturity which implies many of these digital health solutions may not be available today, despite the thriving ecosystem of digital health solution providers including startups.
Recognizing the challenges of developing and customizing point solutions for a wide range of use cases, larger technology firms have developed health cloud platforms and are offering the platforms to end clients and the developer ecosystem to build “last-mile” digital health applications on the platforms.
The next stage in this process is prioritizing and sequencing the roadmap for implementation. A digital transformation framework such as the one above is a useful guide.
The prioritization matrix is a useful guide to communicate with stakeholders involved in the implementation of a digital roadmap. In addition to providing clarity on digitalization priorities, it is helpful as a tool for planning and budgeting for the necessary investments.
The prioritization matrix also serves as a useful portfolio management tool, helping the healthcare enterprise understand the scale and scope of the initiatives, investment allocations, risk levels and payback periods.
(Read our paper: Evaluating health clouds: a primer)

Phase 3: Operating model definition and technology platform selection
The target operating model of a digital transformation program is an essential determinant of success. There are three basic models for enterprises to choose from:
- Centralized
In the centralized model, the digital function and resources are organizationally structured as an operating unit such as a Digital Center of Excellence (COE). The COE drives the execution roadmap, controls funding, and drives policy. This approach can deliver the most optimal use of resources and drive rapid enterprise-wide adoption; however, decision making can be slow and departmental priorities may be neglected. - Decentralized
In the decentralized model, individual departments or functions autonomously drive digital transformation. This approach delivers near-term results. It, however, can result in operational inefficiencies and higher overall costs through duplicate spending and the absence of scale economies. - Hybrid
As the name suggests, a hybrid model combines elements of both centralized and decentralized approaches. This approach is often an acceptable compromise in large health systems where multiple initiatives may already be underway at departmental and functional levels. A hybrid approach can deliver the benefits of a centralized policy, technology selection, and architectural standards while maintaining the autonomy and agility of individual groups.
Implementing a digital strategy: an ecosystem approach
The target operating model of a digital transformation program is an essential determinant of success. There are three basic models for healthcare enterprises to choose from:

It takes a village, as the saying goes. Digital transformation in healthcare requires an ecosystem of strategic partnerships.
The choice of partners could also determine if any of them could be a lead provider and take on the role of “ecosystem integrator.” The digital transformation framework above is used to understand and categorize solution providers.
Many technology providers, especially in the Custodian and Enabler categories, are expanding their range of offerings, on their own or through ecosystem partnerships, to increase their coverage of the needs of a digital transformation program. Thus, an Epic might focus on its MyChart feature to become the primary choice for patient access solutions while a Microsoft Health Cloud might focus more on attracting the developer ecosystem to build solutions on the Microsoft Health Cloud platform.
The Arbitrageurs may include an AWS that brings sheer scale to deliver cloud computing capacity at a fraction of the costs for an enterprise data center. The category also includes consulting firms who may leverage labor cost arbitrage with offshore development centers to deliver services at lower costs. The Innovators are typically firms in the startup ecosystem that are developing new solutions for previously underserved needs, and in some cases reimagining the way existing needs are being served currently.
For healthcare enterprises, there is a yet another choice; build out an in-house development capability, to leverage existing functionalities in their EHR systems as a default choice, and selectively integrate promising startups (while taking equity stakes in some or all of them).
The models will vary based on the enterprise. Some, such as Intermountain Health, have purposefully created stand-alone entities to deliver digital health solutions, whereas others, such as Partners Healthcare and Cleveland Clinic have active innovation programs to identify and nurture promising startup ideas, both within and outside the enterprise. Others, like Kaiser Permanente, have set up sizeable venture capital funding arms that make significant investments in digital health startups.
Regardless of the approach, a fundamental principle in digital transformation is that it’s not about the technology. Digital is more about reimagining experiences and processes using technology and is ultimately about enabling business strategy.

Summary and recommendations
- Digital transformation in healthcare often begins as a departmental initiative in large multi-hospital systems. While this is an excellent approach to experiment with innovation, a significant barrier to increased adoption is the lack of resources and executive-level sponsorship for enterprise-level deployment. This can lead to sub-optimal use of the technology, and a failure to tap into learnings from across the enterprise.
- The technology solutions landscape for an enterprise digital platform is not mature, and no single platform can meet all the digitalization needs of healthcare enterprises substantially. This requires a best of breed approach that creates governance and technology integration challenges. One of the significant challenges with this approach is to ensure that systems integrate and interoperate with each other to support digital transformation.
- Technical debt accumulated over the years can divert scarce resources from innovation and digital transformation towards addressing infrastructure shortcomings and application upgrades.
- Despite the high activity levels in the digital health startup space, the number of viable and proven “last mile” solutions for developing engaging and efficient patient and caregiver experiences is relatively limited. Many digital health startups lack resources as well as a critical mass of live customer deployments, which make it challenging and risky for healthcare enterprises.
- Digital health solutions need significant customization and often lack robust integration with EHR and other systems. It becomes incumbent on the healthcare enterprise to invest in configuring the solutions for the enterprise’s needs and in building an API infrastructure to integrate with systems of records.
- Many digital health programs lack a reimbursement model which make it harder to justify the investments. In such cases, the returns must be often computed in terms of strategic and intangible benefits with a long-term view.
Digital transformation is primarily a cross-functional business initiative that requires a tremendous culture change. While CIOs often lead digital transformation in healthcare, it is not an IT initiative per se and the buy-in of multiple stakeholders, especially among the caregiver community, is critical for success.
For additional insights, please visit our page on healthcare digital transformation.





